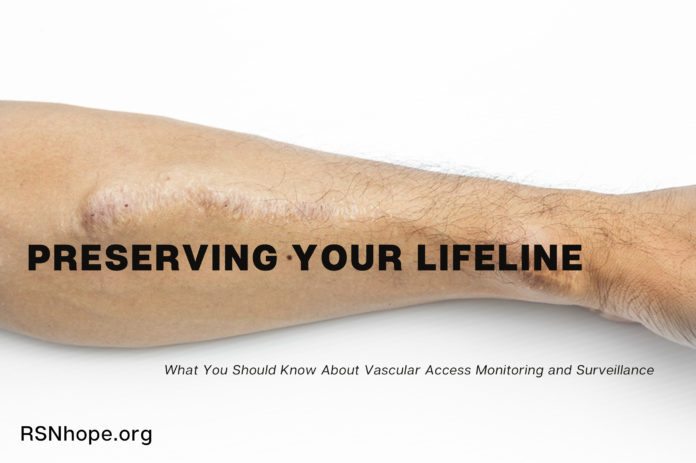
As a person using a graft or fistula for dialysis, one of your highest priorities for maintaining your health and well-being is to make sure that your vascular access is working properly. Problems with your access can decrease the effectiveness of your treatments and lead to hospitalization or loss of your access. What can be done to help keep your access working properly?
The most important issue in access care is the detection and treatment of hemodynamically significant stenosis, or narrowing of the blood vessel by at least 50%, and repair of the access to return it to full function. Most people have some narrowing in their blood vessels, but it can cause serious problems for a dialysis patient when the narrowing occurs in the dialysis access.If a significant stenosis is not treated, it may cause the access to clot off. If your access clots, a declotting procedure, called a thrombectomy, needs to be performed. Thrombectomies can be complicated procedures, and the results are not always successful, so the access might fail anyway.The National Kidney Foundation Kidney Disease Outcomes Quality Initiative (NKF-K/DOQI) Clinical Practice Guidelines outline certain procedures that your dialysis center should be performing to identify the development of hemodynamically significant stenosis. They include procedures for monitoring and surveillance.
Monitoring Your Lifeline
Vascular access monitoring is a physical examination of your access site to detect problems. This monitoring can be done by your caregiver in several ways. One way is looking at your access site for changes such as redness, swelling, or bruising. Another way to monitor is feeling your access and noting any changes like a decrease in the pulsation or warmth. Listening to your access with a stethoscope and noting any changes in the way it sounds is also a form of access monitoring.Your access should get a mini-physical exam each time you have a treatment, when your needles are placed. At least once a month, you should have a complete physical exam done on your access by a member of your medical team. If any significant changes are found, you may need to go and have your access looked at by a surgeon or radiologist.
Surveillance
Vascular access surveillance is periodic testing of your access site that may require special equipment to perform. Abnormal results may indicate a problem with your access.There are several surveillance methods that are acceptable, according to NKF-K/DOQI. One method involves observation, documentation, and tracking of physical symptoms such as:
- Persistent swelling of the access arm;
- Collateral vein development;
- Prolonged bleeding after treatment; or
- A change in the pulsation of your access site.
Direct or derived static pressure readings may be used to monitor for an increase in pressure in the access because increasing pressure can indicate a problem with your access. This test is done by making calculations based on information from your treatment record. You may not even be aware that this method of surveillance is being done because it generally does not affect your regular treatment.
Other acceptable surveillance methods that require additional equipment to perform include duplex ultrasound, measuring recirculation using a non-urea-based dilutional method or ultrasonic dilution for direct flow measurements. You will typically know if these methods are used because a caregiver will need to be present to do the test or you will have to make an appointment to have the testing done outside of your normal treatment.
Evaluation and Treatment
When you have abnormal monitoring or surveillance results, you may need to see a surgeon or interventionalist to find out what is causing your readings to be out of range. A single, isolated abnormal reading should not prompt a referral. Instead, the center staff should be watching the trend of the test results because trend analysis detects access problems more accurately. Persistent abnormal results also indicate that your access should be evaluated.
When you are referred for additional testing, the evaluation is done by fistulogram, which is an X-ray picture of the access after a dye is injected. If narrowing of the vessel by at least 50% in diameter is found, a procedure called angioplasty will be done to open the vessel back up. If the problem cannot be treated by angioplasty, a surgical revision may be necessary to repair your access.
Why Are Monitoring and Surveillance So Important?
Monitoring and surveillance usage helps your caregiver make sure your access is working properly and alerts him/her to problems so your access can be repaired and to prevent it from clotting. If your access clots, there is a greater chance that you could lose the access than if it had been treated by angioplasty before a clotting event.
Ask the staff at your center what type of vascular access monitoring and surveillance they are using for you. Loss of your access can lead to hospitalization for a new access creation and placement or even death if you have no other available access sites.
Remember that your vascular access is your lifeline!
What Can You Do to Help Keep Your Access Working?
Here are a few things you can do to keep your dialysis access healthy and in proper working order:
- Report any changes you notice in your access to your nurse, doctor, or technician.
- Check your access thrill/pulse daily.
- Ask if your center has a Vascular Access Monitoring and Surveillance program. If it does, ask about your results.
- Make and keep appointments to have your access checked if you have abnormal monitoring or surveillance results.
- Protect your access. Keep it clean, and don’t let anyone other than dialysis-trained personnel use it.
- Make sure your access site is used only for dialysis and that no one puts a blood pressure cuff on your access arm.
- Be careful not to bump or cut your access site.
- Don’t wear tight clothing or jewelry over your access site.
- Don’t sleep with your access arm under your body or head.
- Don’t lift heavy objects or put pressure on your access arm (i.e., grocery bags, etc.).
Conclusion
The experts agree that the best access for hemodialysis patients is an arteriovenous (AV) fistula, which is a vein that is enlarged because it has been connected to an artery. A fistula allows blood from the artery to flow into the vein. The higher blood pressure in the artery forces blood into the vein and safely enlarges the vein, creating a good site for the large needles needed for dialysis treatments to be inserted. The preferred first location for a fistula is the forearm.
Fistulas are considered to be the “gold standard” for hemodialysis access. They last longer, need fewer repairs, and are associated with lower rates of infections, hospitalization, and death than other types of accesses.
Recognizing the fact that fistulas are the best and safest kind of vascular access for dialysis treatments, the Centers for Medicare & Medicaid Services (CMS), in conjunction with the federally-mandated End-Stage Renal Disease (ESRD) Networks, dialysis providers, clinicians, and patients, established the Fistula First initiative to promote the creation and use of an arteriovenous fistula as the first hemodialysis access and to increase the number of fistulas being placed for existing hemodialysis patients. The target is to have fistulas placed in at least half of new dialysis patients with a long-range goal of maintaining fistulas in 40% of eligible patients who remain on dialysis.
The goal is for every kidney patients to be evaluated for fistula placement before they begin dialysis treatments. There are some excellent diagnostic tests such as vessel mapping that could identify vessels for creating a fistula. This procedure will also let you know whether or not you are a fistula candidate. CMS has set a new goal for fistulas–66% of hemodialysis patients should receive their treatments through an AV fistula by June 30, 2009.
The bottom line goal of Fistula First is to improve and promote the quality of care and quality of life for patients living with kidney failure by placing the best access that has the least complications.
Glossary
Angioplasty: The repair of a blood vessel abnormality.
Direct flow measurement: A testing method that determines the amount of blood flowing through a system.
Direct static pressure: Pressures measured directly at the site of cannulation in the arterial and venous segments of the graft or fistula using a pressure-measuring device.
Derived static pressure: Calculated by using the venous pressure readings from the machine, blood flow, coefficients sets (based on type of machine, needles and bloodlines), MAP, and hematocrit/hemoglobin.
Duplex ultrasound: Combines Doppler ultrasound and imaging to provide diagnostic ultrasound used for quantitative color velocity imaging, also referred to as Doppler sonography. Or a direct flow ultrasound measurement with a color image.
Fistulogram: An x-ray examination of the fistula or graft.
Hemodynamic: The status of the body’s blood system or something that relates to the physical aspects of blood circulation.
Interventionalist: A medical specialist who treats access problems.
Pulse: The rhythmic contraction and expansion of the arteries/access with each beat of the heart.
Stenosis: A constriction or narrowing of a duct, passage, or blood vessel.
Thrill: A vibration or buzz that can be felt in the graft or fistula.
Thrombectomy: Surgical removal of a blood clot.
Ultrasonic dilution: A type of direct flow measurement made by administering saline and taking measurements of the flow in the bloodlines going forward and in reverse.
 About the Author
About the Author
DeLynn Huff, BS, RN, CNN, is the Clinical Implementation and Quality Coordinator for Vasc-Alert, LLC, West Lafayette, IN. Her clinical experience includes 14 years in the hemodialysis setting, where she has worked as a staff nurse, clinical educator, and clinical manager. DeLynn has been a Certified Nephrology Nurse since 1999.
07/01/2007
Web ID 390